The kidneys are two reddish-brown, bean-shaped organs that are around the size of a fist. They are placed on either side of your spine, directly below the rib cage. Kidneys are very important organs in human body as they carry out some of the most important function including:
kidney transplant is a surgical procedure that involves implanting a healthy kidney from a living or deceased donor into a person whose kidneys are no longer functioning correctly.
In order to survive, people with end-stage renal diseases have to get waste removed from their bloodstream via dialysis or a kidney transplant.
When kidneys lose their ability to filter properly, harmful levels of fluid and waste accumulate in the body, which can lead to an increase in the blood pressure and result in kidney failure (end-stage renal disease). End-stage renal disease occurs when the kidneys have lost about 90% of their ability to function normally.
Common causes of end-stage kidney disease include:
A kidney transplant is a surgical procedure, frequently used to treat chronic kidney disease and renal failure. It can help patients with Kidney failure live longer and healthier lives. Kidney transplantation can result in:
However, for certain patients, a kidney transplant may be riskier than dialysis. The following conditions may exclude you from getting a kidney transplant:
Ther are two type of organ donor:
Receiving a kidney from a family member is a safer alternative since it lowers the danger of the body rejecting the kidney and allows you to avoid the years long waiting list for a deceased donor. When you get a kidney from an unrelated donor, your body is more likely to reject it.
Please note that only 'near relative' such as spouse, parents, siblings, grandparents, and children of the recipient can be living donors for kidney transplant as per the law in several countries.
If a compatible living donor is not found, your name will be added to a waiting list for a deceased-donor kidney.
Here are brief details of what happen before, during and after Kidney transplant.
Once a kidney transplant is recommended by your doctor, you'll need to choose a transplant centre where you will be evaluated to see if you meet eligibility requirements of that particular transplant centre. As a result, you may need to be evaluated to determine whether you are healthy enough to have transplant surgery, whether you have any medical conditions that could interfere with the transplant, and whether you are willing to take the necessary medications. After the evaluation is done, you will undergo specific tests and procedures, which includes:
Doctors will evaluate the results of your tests to determine the severity of your illness and the urgency with which you require a kidney transplant.
Doctors look into following factors to identify a suitable and compatible kidney:
Having a compatible blood type reduces the likelihood of your body rejecting the donor kidney. Tissue Typing evaluates genetic markers that improve the chances of the donated kidney lasting a long period. An excellent match implies your body is less likely to reject the transplant. Crossmatch test involves mixing a small sample of your blood with the donor's blood in the lab. The test determines whether antibodies in your blood will react against specific antigens in the donor's blood. A negative crossmatch means they are compatible and your body isn't as likely to reject the donor kidney.
IIt is preferred for donor to have compatible blood group (the same blood group that recipient has), but now a day’s incompatible blood group transplant (transplant with different blood group) is also possible. However, in this type of transplant, antibodies in the patient against donor blood group has to be removed through plasmapheresis/immunoadsorption/ medication. So, this type of transplant is more costly as compared to transplant with same blood group. The donor and recipient will have to undergo detailed tests, which could take 7-15 days (depending on what is found on investigations), prior to transplantation. The Transplantation can be done if the recipient and donor are found to be fit after these tests. Incompatible kidney Transplant is called ABO-incompatible kidney transplantation (ABOi LT) as well.
If you are getting the organ from a living donor, your doctor can plan the transplant in advance. If, on the other hand, you are awaiting a deceased donor who is a close match for your tissue type, you may need to rush to the hospital at any time.
When you arrive at the centre, you will be asked to provide a blood sample for an antibody test. If the test result is a negative crossmatch, you will be cleared for surgery.
Because general anaesthesia is used during kidney transplant surgery, you will be sedated throughout the procedure.
During this type of procedure, surgeons place a number of tubes and IVs (Intravenous Catheters) in your body to perform specific function (such as delivering fluids and medicine, monitoring heart and blood pressure, taking blood samples, helping your breath by ventilator tube, drain blood and fluid from around your kidney and draining urine etc.) while you are unconscious. The tubes will be left in place for a few days following your surgery.
The surgeons will visually inspect the donor kidney before implanting.
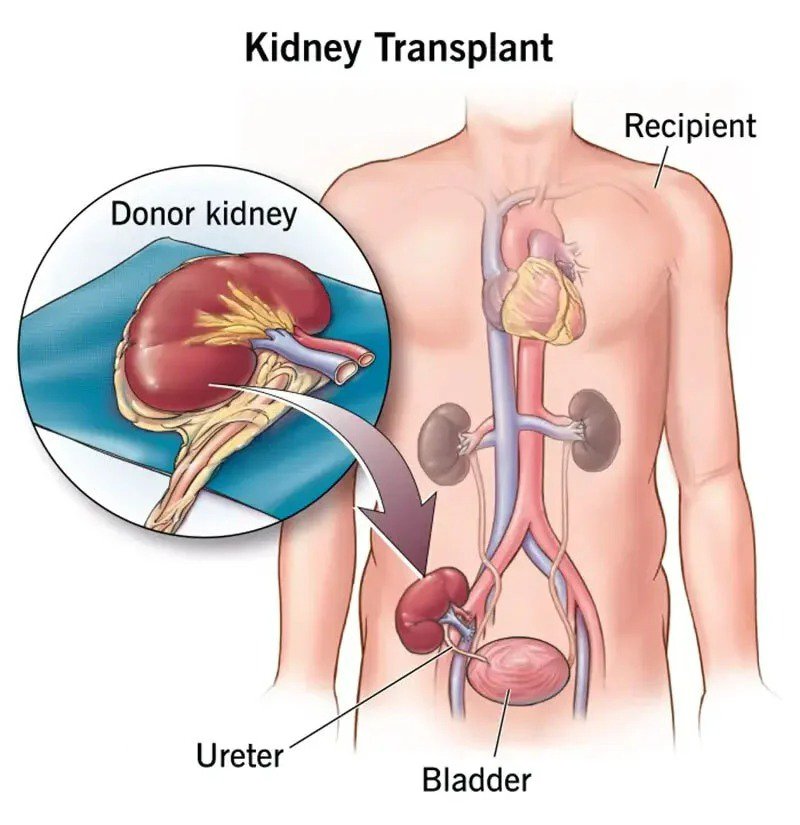
Once you are asleep under general anaesthesia, the surgeon will make an incision in your abdomen, and place the donor kidney inside. A left donor kidney will be implanted on your right side; a right donor kidney will be implanted on your left side. This allows the ureter to be accessed easily for connection to your bladder.
After which, surgeons will connect all the arteries and veins from the kidney to your arteries and veins. This will let the blood start flowing smoothly through the new kidney soon. The blood flow through these vessels will be checked for bleeding at the suture lines.
Your doctor will next connect the ureter of the new kidney to your bladder, allowing you to pee normally. Your original kidneys will not be removed from your body unless they are producing difficulties.
If you are receiving your new liver from a living donor, the surgery must be planned ahead of time in advance. The donor is first operated on, and the kidney for transplant is removed from the donor’s body. Following that, the donated kidney is implanted in recipient’s body.
After the new kidney is in place, the surgeon closes the incision with stitches and staples. A drain may be placed in the incision site to reduce swelling. After that, you are taken to the intensive care unit to begin your recovery.
After your procedure, you may need to stay in the intensive care unit for a few days. Medical personnel will need to keep an eye on your condition and look for signs of complications. They may conduct some tests as per the requirement.
Your doctors will also prescribe antibacterial, antiviral, antifungal and other medications to prevent your body from rejecting the new kidney and any kind of infections or any further complication as after such surgeries the body become more vulnerable to infection.
After a successful kidney transplant, your new kidney will filter your blood, and you will no longer need dialysis.
It is important that you take all of your medications exactly as prescribed by your doctor, since even if you miss a few doses, your body may reject your new kidney. If you notice any negative effects from your drugs, you should inform the transplant team right away.
A kidney transplant is of some potential risks, and as with any major surgery, there are various risks involved. Among these dangers are:
Despite these risks and complications, a kidney transplant is still seen to be the best option for someone suffering from chronic kidney disease or end-stage renal disease. Following the treatment, patients may be required to take anti-rejection medicine for the rest of their lives. As a result, it is essential to talk with your doctor before proceeding with a transplant.
Please note that this is general information about the kidney transplant surgery, some details may change, if have any query please reach out to your liver transplant surgeon.